Reticulocyte Count
Why they are more important than just classifying anemia?
Reticulocytes: what are these?
- Reticulocytes are immature red blood cells that remain in the bone marrow for 24–48 hours before being released into the circulation, where they reach full maturation after a further 24-48 hours.
- Key features of reticulocytes are:
- They are larger than mature red cells;
- They contain less hemoglobin than mature red cells.
- They develop into mature erythrocytes when hemoglobin synthesis is completed and the cell size has reduced to that of the adult.
- Since Reticulocytes are the youngest erythrocytes released from the bone marrow into the blood, their hemoglobin content reflects the amount of iron available for hemoglobin production in the bone marrow.
Historically, assessment of reticulocytosis was significant only in cases of anemia, but recent studies proved otherwise.
Why do we care so much about assessment of reticulocytosis?
- Reticulocytosis help the clinician to differentiate regenerative from non-regenerative anemia (the cornerstone for DDx of anemia):
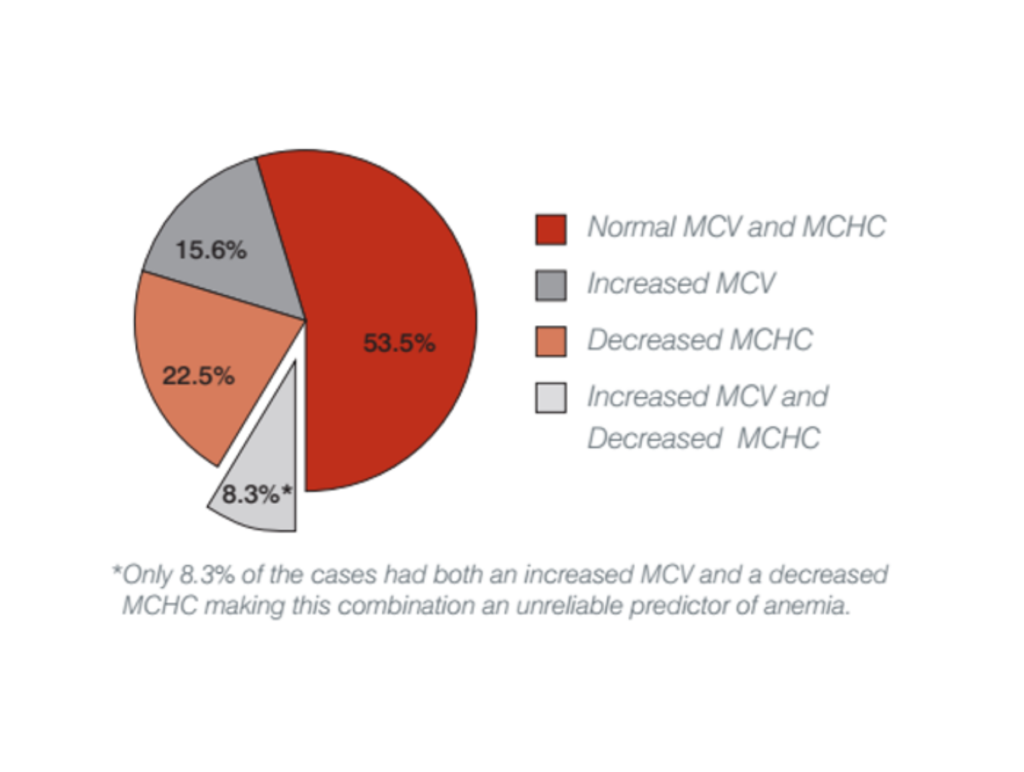
- DiNicola et al. reported that only 8.3% of blood samples of 6752 dogs with regenerative anemia had both increased MCV and decreased MCHC despite the principle that regenerative anemia has increased numbers of macrocytic and hypochromic RBCs, which is true and important in diagnosis.
- Historically, assessment of reticulocytosis was significant only in cases of anemia, but recent studies proved otherwise. Reticulocytosis may serve as an early alarming system for more serious conditions:
- Reticulocytosis without anemia can be a key indicator that the bone marrow is responding to a need for increased red blood cell production (compensated blood loss, hemolysis, hypoxia (determining the underlying cause will require further investigation, but early detection provides the best chance for early treatment and better outcomes for patients).
- While RETICs measure the quantity of new RBCs, RETIC-HGB reflects the quality-generally related to the amount of iron available during the formation of these cells; the most common causes of low RETIC-HGB are blood loss and inflammatory disease, which both lead to decreased iron availability for RBC production; a low RETIC-HGB result may indicate serious underlying disease before an increase in RETICs or anemia, warranting further exploration.
What could CBCs lacking reticulocyte parameters miss?
A recent study of 1 million canine CBCs found that almost 1 in 5 nonanemic patients had changes in their reticulocyte parameters:
- Six percent had no anemia, but a high reticulocyte count.
- Twelve percent had no anemia or reticulocytotic , but had low RETIC-HGB concentration.
This research indicates that reticulocyte parameters should be evaluated with every CBC: Don’t wait for the anemia to develop. Not all CBCs include reticulocyte parameters. When choosing a CBC, look for those that automatically include reticulocytes.

